Shortly about Eyes and Vision
The eyes and sight of a baby we experience very important. Intensive eye contact with a newborn baby connects the adult with the infant and the “social smile” that develops in a few weeks is one of the most important behaviors that strengthen the bonding between an infant and parents.
Copying of facial expressions can be present quite early. Infants born without much stress can be very active already during the first few days, watch’s the faces in front of them, especially the mouth and even copy a few facial expressions.
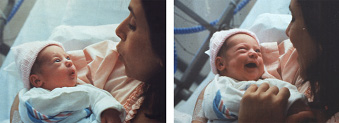
How can you prevent or decrease visual impairment by observing your infant’s visual behaviors?
Most infants and children grow up with normal eyes and vision and do not need anything else but the follow-up that they reach the usual milestones of vision development at the usual ages. The most common cause of impaired vision in children is Amblyopia, “lazy eye”. It is caused by disturbance in use of an eye during the sensitive period. The disturbing factor may be
- a transient swelling of an eye lid or patching because of a corneal wound - therefore after such a period of disturbance in the development of binocularity, especially during the first year, the occluded eye needs to be trained until it functions as well as the other eye, i.e. fixation has become equal to that of the other eye
- cloudy media, examination of red reflex is the important test to detect cataract but also corneal cloudiness and/or vitreous changes - rarely a retinoblastoma
- strabismus, usually first transient then constant - constant strabismus should always be referred without delay and after 6 months of age also transient strabismus needs to be assessed by a pediatric ophthalmologist without delay. If treatment is started before the angle becomes constant, binocularity may be easier to regain. Cover test and Hirschberg's test are the tests used in screening.
- unequal refractive power causing blurred image in one eye - detectable as a difference between the eyes in the child's behavior during monocular tracking of a small target. Demonstrate to the parents the use of the cover test so they can observe development of vision of both eyes separately in play situations. (See "Info for parents")
 Visual impairment of both eyes, may be anterior, due to changes in the eyes and/or anterior visual pathways, or due to damage in the posterior pathways, posterior to lateral geniculate nucleus (LGN), in the primary visual cortex (V1), associative cortical functions or subcortical visual functions. A great majority of cases are congenital and thus can be diagnosed early when the infant has roving eye movements, nystagmus and does not develop normal eye contact. Later during the first year, infections, accidental and nonaccidental traumas and tumors may cause vision loss. More than 60% of visually impaired infants have at least one other impairment or chronic illness.
Visual impairment of both eyes, may be anterior, due to changes in the eyes and/or anterior visual pathways, or due to damage in the posterior pathways, posterior to lateral geniculate nucleus (LGN), in the primary visual cortex (V1), associative cortical functions or subcortical visual functions. A great majority of cases are congenital and thus can be diagnosed early when the infant has roving eye movements, nystagmus and does not develop normal eye contact. Later during the first year, infections, accidental and nonaccidental traumas and tumors may cause vision loss. More than 60% of visually impaired infants have at least one other impairment or chronic illness.
Since vision is the main avenue of interaction and learning, it should be remembered as one of the important causes of deviations from normal development. If early interaction is not developing normally, the possibility of sensory impairment and deprivation as the cause should be carefully investigated. Both vision and hearing need to be assesed during clinical examinations and functional vision testing performed by an early intervention specialist.
An infant may have normal eyes but delayed development of accommodation, instable fixation of gaze or central scotoma in the visual fields, which prevent the infant from having normal eye contact with the parents. The child may not have delayed general development when the abnormal eye contact is noticed. If the parents are given guidance and support and if the infant receives compensatory information in communication, general development is not likely to become delayed.
Healthy children rarely have poor accommodation whereas it is common among infants with Down Syndrome, hypotonia and cerebral palsy. Poor accommodation can and should be compensated with "reading lenses", near correction, to give the infant clear images on the retina. These infants and infants in families with large refractive errors or a history of amblyopia, "lazy eye" need to tested by a paediatric ophthalmologist because there are no tests that would reveal irregular refractive errors or poor accommodation in your office.
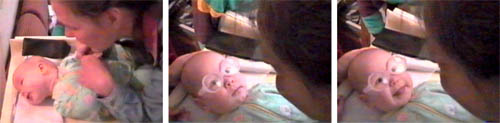
This otherwise healthy infant had been diagnosed as having infantile autism because she turned her face away from an adult approaching her. She was found not to accommodate, not even to very high contrast fixation targets. When the failing accommodation was compensated with near correction lenses, she looked greatly surprise for a few seconds and then had a normal social smile for the first time.
Premature infants and infants with asphyxia during intrauterine development or after birth are in danger of having losses of isolated visual functions: recognition of faces or facial expressions, perception of objects in motion or spatial relationships or difficulties in eye-hand coordination. If not diagnosed early, the losses of visual functioning interfere with early interaction and social development. These children need to learn to use techniques of blind persons in functions where they cannot use vision. This is an area of special education that is not well known, so you need to work together with an experienced paediatric neuropsychologist, an occupational therapist and a vision teacher who are accustomed to examine blind children. Even in the school age these children are a challenge because it is difficult to get acceptance by the school authorities that an obviously sighted child needs teaching with blind techniques in some areas.
Children with intellectual disabilities are more likely to have large refractive errors than children with normal early development. Therefore their eyes need to be examined early.
Deaf children need to be examined for inherited retinal degenerations, most often retinitis pigmentosa. Usually RP does not cause any symptoms during the first year of life. In some children decreased night vision can be observed already during the first or second year. A deaf toddler who turns on lights, clings to the parents in dim light but runs independently in day light, should be assessed. Follow-up of cone cell adaptation by measuring the speed of adaptation with the CONE Adaptation test (Good-Lite) allows an early diagnosis of a change in visual adaptation.
Consultations are your important support to confirm your observations. You should receive information on following important findings:
- description on the visual behavior of the infant
- structure of the eyes and optic nerve heads
- oculomotor functions
- refractive power
- power of lenses if glasses were prescribed
- diagnosis, if known, or a likely cause of the visual impairment
This information should be the result of all consultations. If the ophthalmologist is accustomed to work with the early intervention specialists, there is also a discussion on the effect of visual impairment on
communcation/early interaction
motor development
development of spatial concepts and object permanence
When this kind of information is available it is possible to make plans for early intervention with the local early intervention specialists and vision teachers. Since these children so often have other impairments and diseases the role of the local paediatrician as the coordinator of treatments and habilitation activities is central. The local team can best support young parents in the care of their child, be it "simple" patching of a leading eye and training of the amblyopic eye or complicated care of contact lenses or intensive training of vision in both eyes.
Early intervention is crucial in all cases of visual impairment, which often causes a "developmental emergency" situation because vision is so central in early development, especially in early interaction and early motor development.
If normal eye contact does not develop the parents need counseling and advice how to communicate with their baby. Otherwise communication is experienced so distressing that it is avoided, yet a visually impaired baby needs more interaction than a baby with normal sight.
If vision does not entice the infant to lift the head, strength of the arms and schoulders does not develop and crawling is delayed. Special play situations to train head control require an early intervention specialist who teaches them to the parents and care takers in day care.
 |
 |
Bringing hands to midline (Fig.1) is an important motor function and an important step in the development of spatial concepts. "Little room" (Fig.2) is an inexpensive plaything to help a visually impaired infant in the development of spatial concepts. Without good spatial concepts orientation in space becomes problematic. When a visually impaired child learns to walk, motor training is not completed. Training of orientation and mobility techniques then starts with an instructor of these special techniques, with or without the white cane (Fig.3).

Fig.3