Interpreting During a Medical Examination
The use of an interpreter during the medical examination causes problems because of the very technical nature of the vocabulary used by doctors. The interpreter may be fluent in many areas of communication and yet have considerable difficulty in trying to carefully convey the medical information from one language into another. The difficulties of translation from one spoken language into another spoken language are well known and appreciated, whereas the difficulties related to interpretation from spoken language into sign language, and vice versa, are much less well known. A patient may be familiar with the meaning of a medical idiom in his mother tongue, the sign language, but may be lost if the corresponding idiom is "translated", word for word.
Because of the misconception that sign languages are visually presented, simplified spoken languages, the translation is often thought to happen without the usual problems of interpretation. Translation between spoken language and sign language requires the same special skills needed for translation from one spoken language into another. Not everyone who knows sign language can function as an interpreter.
In any communication situation that involves an interpreter there are several different types of communication going on simultaneously. This is depicted in Figure 4.B where the major part of the communication is transferred by the interpreter but a significant part happens directly between the patient and the doctor through body language and facial expressions (dashed line). This direct communication helps the doctor sense how far the interpreter has come in signing and how well the patient may understand the information.
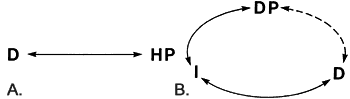
Figure 4. A. Communication between a hearing patient and his doctor is direct and can continue during the different tests. B. Communication between a deaf patient and his doctor is mostly conveyed by the interpreter (solid line). Some of the communication is direct (dashed line) but even this is interrupted during the measurements. HP (=hearing patient), D= doctor, DP= deaf patient, I = interpreter.
In many tests, communication through an interpreter is slower than spoken communication because it is interrupted each time the patient looks at the test. The test instructions must be explained before the test begins and the test may be interrupted again if the patient does not seem to have fully understood the explanation. The interpreter must usually wait for a moment in order to get an idea of what the doctor is going to ask next, and therefore the interpretation is not simultaneous but slightly delayed. The delay in interpretation decreases when the doctor learns some basic rules of sign language and the interpreter becomes familiar in working with the doctor.
Sign language is very rich in expressions but not in specific signs for a number of concepts that we use during the assessment of health and diseases. These concepts must each be introduced and often explained, all of which requires additional time. If the interpreter knows the patient and his linguistic capabilities and knows the contents of the examination and phrases used by the doctor, interpretation is considerably facilitated, since the interpreter can prepare different ways of expressing certain questions that otherwise would not be understood by the patient. The more often the interpreter and the doctor work together the more they learn about the difficult moments in their communication, and thus the less frequent these moments become.
The use of an interpreter should never become a barrier between the patient and the doctor. Even if the information goes via the interpreter, the doctor must always address the patient and not the interpreter. It is inappropriate to say "Tell him . . ." The discussion with the deaf patient should have the same character as that with a hearing patient, even if it is slower. During the discussion it often happens that the patient looks at the doctor when the doctor begins to speak or keeps looking at the test when additional instructions should be given. Since the patient is usually out of reach of the interpreter and within reach of the doctor it is the doctor's responsibility to guide the patient's attention to the interpreter, especially in cases when the patient's small visual field makes it impossible for the interpreter to catch the patient's attention.
Although interpreters are asked to function as totally impartial 'connecting cables' between the deaf person and the doctor, they share the emotional stress of patients. If the doctor is rude or nonchalant, the interpreter has to convey the attitude even if it is apparent that this will hurt the patient. By learning to appreciate the work of interpreters, we may learn to express ourselves more gently.
A visit to the ophthalmologist's office is often more stressing than other health visits. Deaf persons value their sight even more than hearing people do and blindness is often seen as being worse than death. Therefore, a visit to an ophthalmologist, especially when vision is impaired, may be emotionally difficult. The patient's attention may be affected by worries and he may be very sensitive to the way the communication is handled. A person's adjustment to the loss of previous visual capabilities is strongly affected by the attitude of his ophthalmologist. Rehabilitation starts, or is affected negatively, in the office of the first doctor who tells the patient about the impending visual impairment, and it continues to be affected by every subsequent contact.