Visual Acuity
Refraction
Before visual acuity can be measured we firstly have to measure refraction. Again, it is best to use either the interpreter or another person signing as the fixation target in order to maintain communication, if the patient sees with both eyes.
In a number of cases, objective measurement of refraction is difficult, unreliable, or impossible because of distortion of the image in the optical media, uncertainty of retinal location used for viewing, miosis or other causes that block the passage of the beam. In these cases, subjective refraction should be mastered by the examiner.
Uncorrected large refractive errors are common among hearing and visually impaired persons, especially when they have developmental delay. By large refractive error, I mean sizable errors of up to 10-15 diopters. If the first +10 diopter lens placed in the trial frame does not change the near point, you may need two more in order to bring the image within near vision. Likewise large uncorrected myopia is quite common. If the patient cannot answer during testing with optotype tests and the best subjective correction, grating acuity tests may be used.
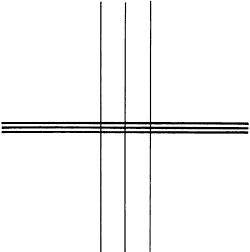
Figure 9. A simple cross for subjective assessment of astigmatic errors.
Once the near point has been found, the presence of astigmatic error may be found using a simple picture of a cross that the patient himself can move so that first the lines in one orientation and then the lines in the other orientation are sharp. A measure stick with dioptric markings facilitates the estimation of refraction. This very old technique of measuring astigmatism is still useful when objective measurements do not work.
Many patients use one area of the retina for viewing in near vision tasks and another for distance vision. The importance of astigmatic correction varies. It is often surprising to notice that the patient may be able to reliably demonstrate the presence of astigmatic error when tested with the cross, yet when reading he does not notice a difference when the axis of cylinder is changed 90 degrees. Unnecessary astigmatic corrections should be avoided.
The question "Which is better, the first lens or the second lens?" used during subjective refraction is confusing in sign language because the sign "better" is a derivate of the sign "good". If neither of the two alternatives is "good", how can the patient determine which is "better"? After such a question the answer is usually "Neither", after which the next question is "Any difference?". It is often possible to adjust the correction of a hearing impaired patient as finely as with hearing, visually impaired patients. In many cases, even the cross cylinder can be used with great exactness. The two choices have to be signalled by the examiner to the patient tactually, for example, one finger placed on the hand of the patient meaning first alternative and two fingers for the second alternative.
Optotype tests
The group of deafblind patients covers all age groups and all communication levels, and thus we have to be prepared to use all available tests and to create new tests and testing situations when nothing seems to work. This chapter will deal with the usual examination in the office. The assessment of vision in severely disabled children and adults will be discussed in separate chapters.
Visual acuity tests using optotypes are linear tests, single symbol tests, or tests with more crowded symbols. Low vision clinics and individual eye specialists serving the visually impaired patient are now quite modern (NOTE: this was written in 1988) in their visual acuity testing, i.e. they use new charts designed according to the principles published by Bailey and Lovie (1976) and recommend by the Consilium Ophthalmologicum (1988). There are now several tests with minor differences in the form of the letters, being the Sloan, Snellen or British letters and paediatric tests for patients who cannot be tested with the letter charts. Projected charts should not be used because the room lights have to be too dim, the difference between the luminance level of the chart and that of the face and hands of the interpreter is too great. Young children and persons with intellectual disabilities start testing with the LEA SYMBOLS® 3D puzzle, preferably weeks before the examination in the doctor's office. Near vision tests recommended for assessment of abnormal vision should be based on the same optotypes as the distance charts and have the same basic layout.
Visual acuity tests are designed for a certain distance. Patients with abnormal vision have varying preferred distances for sustained near work. Therefore the testing of visual acuity should be done at the preferred distance and with the preferred head posture. The visual acuity value is then calculated as a function of distance.
Communication during measurement of visual acuity in near vision is often problematic if the person finger spells the letters close to the test. The interpreter may have to stand up to see the finger spelling. As it is impossible to inform the patient about the test when he is looking at it, I prefer to use a card with which I can cover the lines above or below the line to be read. In this case there is seldom any misunderstanding about what to look at.
Grating acuity
Infants and older patients who cannot answer in optotype tests, can be tested by using small objects or grating targets and observing what is the smallest object or the finest grating that the child can discriminate or shows a response to. These acuity values are different from values measured as recognition acuities with optotypes. In abnormal visual systems, and possibly also in the developing visual system, the ratio between optotype acuity and grating acuity varies greatly (Hyvärinen 1983). Even in a normal visual system the ratio between these two acuity values varies at the different acuity levels (Hyvärinen et al 1987).
Standardized word lists
Reading high contrast print requires recognition of symbols that are closer to each other than symbols in a line test. For children who cannot yet read there is a test with crowded symbols as a part of the LEA-near vision card. For older children and adults we need standardized word lists. In English there is a word list with words of different lengths. Since the words have to be finger spelled, the test situation is quite difficult for the interpreter: the words cannot easily be learned by heart and there is little time to check from a copy of the test. Reception of independent words finger spelled by an unknown person is a very demanding task.
Reading of continuous text
A text used for testing reading ability of a person with low vision should be standardized to be equally difficult throughout each page of the test. Tests for the deaf population should contain words common in "deaf English" and they should have texts at different grade levels.