GLAUCOMA
Glaucoma is a group of diseases that cause loss of visual field because nerve fibers are damaged at the optic disk. In many but not all cases the pressure inside the eye, the intraocular pressure, is higher than normal and causes changes in the nerve fibers of the optic nerve, over a very long period of time. Glaucoma is often diagnosed during health control visit, the person is unaware of the changes in his eyes. There is a more rare type of glaucoma in which the pressure rises acutely causing pain and redness of the eye.
Glaucoma is often difficult to diagnose because there are so many variants of normal structure of the optic disc and sometimes the noticeable changes in the optic disc appear late. An example of these problems is in the following Figure 11.
A 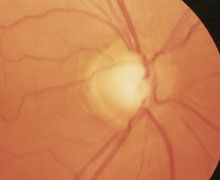 B
B 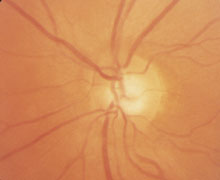
Figure 11. This person was examined more than ten years ago and was found to have optic disc changes in the right eye (A) that were rather typical to glaucoma: enlargement of the optic cup and displacement of the vessels toward the nasal side. The optic disc of the left eye (B) was normal. However, no high pressures have been measured during the past years, the visual fields are normal and the structure of the optic disc has not changed. The question then is: is this a congenital difference or was there one time high pressure or circulatory changes that changed the structure of the optic disc. There is no sure answer and therefore the condition must be followed repeating visual fields and measurement of intraocular pressure.
Even a normal eye has certain intraocular pressure. The pressure varies usually between 10 and 21 mmHg (quicksilver millimeter) and is often highest early in the morning. If the pressure rises or there are changes in the circulation of the nerve head, nerve fiber function becomes disturbed and some fibers die. In the corresponding areas of the visual field small blind patches, scotomas, are found. The areas of loss of vision are first very small and cannot be noticed by the person himself. Therefore it is important that the eyes are controlled by an ophthalmologist regularly when the person is past 50 years.
|
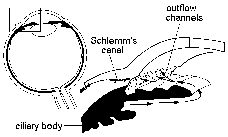
Fig.11c. Intraocular fluid is formed in the ciliary body behind the iris. It flows through the pupil into the anterior chamber. It drains through the small pores at the anterior chamber angle into the veins on the surface of the eye. |
Since the intraocular pressure (IOP) varies even in normal individuals, it is necessary to measure the pressure several times at different hours of the day if one suspects that the pressure might be too high at times.
|
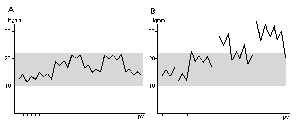
Fig.12. Variations of the intraocular pressure. A.Normal variation. B.Occasional high pressure values. |
|
Mere measurement of the intraocular pressure is not sufficient for ruling out of glaucoma. The eyegrounds, especially the nerve heads, called the discs, have to be examined and the visual fields recorded.
|
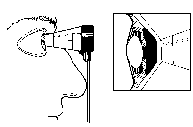
Fig.13. Measurement of the intraocular pressure (IOP). A. Measurement with an applanation tonometer. |
|
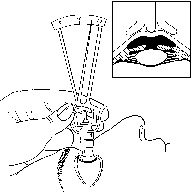
B. Measurement with a Schiotz' tonometer. |
In hospitals and in doctors' offices the IOP is measured with an applanation tonometer. It is a small device that gently touches the cornea. The patient may not notice the moment of measurement because the corneal surface is anesthetized with drops. (S)he sees the blue light approaching, then it stops to touch the cornea and then moves away.
An older instrument is Schiotz' tonometer. The patient lies on his/her back looking at the ceiling, the instrument is placed on the cornea and the pressure is read on the scale. This instrument is sometimes loaned for measurements at home.
Measurement of the visual fields tries to reveal whether there are small poorly functioning areas, scotomas, in the field of vision. The instrument used is called perimeter and the examination is called perimetry. There are many different perimeters. In some perimeters tiny lights appear now and then in different parts of the visual field. When one or more lights appear the patient pressures the button as a sign that he has seen the light(s). In other perimeters the light moves from the edge of the perimeter inwards until it becomes visible. The patient always looks into the central spot of the perimeter. He/she does not move his/her eyes around to find the moving spot.
The anterior chamber angle is examined with a small contact lens that is placed on the cornea. In the contact lens there is a small mirror in which one can see the anterior chamber angle. This contact lens is different from the contact lens that are used instead of glasses (Fig.13c).

Figure 13c. The three mirror lens or the gonioscopy lens (gonio= angle, scopy= to look) can be used to examine the structures in the anterior chamber angle.
There are many kinds of medications used in the treatment of glaucoma, both eye drops and pills. Eye drops that lower the intraocular pressure are powerful medicines. If the drops get into the nose and from there into the stomach some of them may cause disturbance in the functions of the stomach and the gut. They may also cause allergic rhinitis and asthma. Therefore, the drops should be dropped on the conjunctiva of the lower lid. The eye is then closed and the inner corner of the eye pressed gently with paper handkerchief to prevent the drops from getting into the tear channels.
The eye drops should not get on the skin because they may cause excema. If it is difficult to drop one may ask the optician to drill small holes in old reading glasses. The holes are not drilled at the center of the lens, but slightly toward the side. The hole has to be large enough to let the tip of the dropper to go through. Otherwise the drops flow on the glasses. There are special supporting cups available for dropping the eye drops.
If medications do not control the intraocular pressure well enough, laser treatment and several different operations may be considered.
Glaucoma with closure of the anterior chamber angle develops if the iris is pushed forward and blocks the anterior chamber angle. The pressure rapidly rises very high, the eye becomes painful, reddish, vision becomes blurred and the patient often has nausea. The patient needs immediate treatment because the nerve fibers do not tolerate high pressure for an extented period of time.