13. CHILDREN WHO BECOME VISUALLY IMPAIRED AND SEVERELY MULTIHANDICAPPED BEFORE SCHOOL AGE
The number of children who see normally or near normally during the first year of life and then become visually impaired and severely multihandicapped before school age or during the lower grades, is limited. Their assessment resembles assessment of infants because much of the work is done by the care takers, therapists and special teachers. The low vision team can help with the basic clinical information making sure that the anatomy of the eyes and visual pathways is well recorded and described to the people involved with the care of the child and demonstrating the test situations that seem feasible in the beginning and later.
When assessing these children we keep in mind the numerous factors that may affect the child's responses:
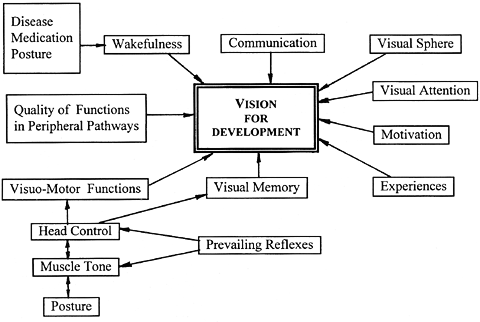
This diagram shows the most important variables affecting an assessment. These children are usually seriously ill, weak and sleepy because of medications. It is wise to inquire when medications are given and chose a time when their effect on wakefulness might be lowest. Often an ophthalmologist or the low vision team members are asked for consultation early in the morning, less than an hour after the child has had his/her largest dose of medicines and is sound asleep. A better time for assessment is during and after the mid-day meal or later in the afternoon. Parents and therapists usually know the best time during the day and are a great help in evaluating the responses.
Communication needs to be at the level of the child. During the first assessment parents demonstrate how they communicate with the child so we can choose a type of communication that the child is accustomed to. This includes all types of communication, visual, tactile, auditory, even smell if we want the child to recognise us later on a special smell.
Visual sphere is one of the first things to observe, because we need to test well within the visual sphere. The space, within which the child uses vision, is dependent on the visual qualities of the object, its movement and its emotional value. A milk bottle with dark stripes on it is recognised at a longer distance than a square or round picture with similar stripes on it. A flickering light is often responded to at a much longer distance than a small flashlight. Parent's face is one of the best objects for testing visual sphere.
Visual attention may be much less on one side of the visual field than on the other or present only in the very middle of the visual field (see the video 'Oona', measurement of visual field during the first assessment). If clinical findings suggest that parts of visual field may be lost or that visual acuity and contrast sensitivity are likely to be poor, we need to use strong stimuli as fixation targets and present them first in the best areas of the visual field.
Oculomotor functions are used as signs of responses. Therefore it is important to know how they are affected and to observe them for some time when the parents interact with the child. If there are abnormal eye movements we must not let them disturb our observations. During presentation of test objects we must remember not to adjust the speed and direction of movement of the test object to the movements of the child's eyes. The object is brought to a point in the child's visual field where it should be visible and them moved in any of the cardinal directions to find out whether it elicits following movement.
Motor problems in arms and hands may make reaching impossible but we might see an intention to move the hand in correct direction. Pathologic reflexes may disturb head movements and may require change of posture and/or support by the child's physiotherapist.
Motivation to participate in the test situation may be low if the child has unpleasant memories of unknown persons causing pain in previous treatments or examinations. Often the child's own therapist is the best person to start the test situation guided by the low vision team.
The first assessment is seldom very successful. We do not yet know the child and the child does not relate to us. Many observations during the first assessment are later found to be interpreted wrongly. This is important to remember and also tell the parents asking them to repeat the test situations together with the therapist to find out how often the response is similar to the response seen during the assessment. Quite often parents or the therapist spontaneously tell that 'this response is not his/her normal response'.
Early intervention should in these cases start during the hospital care, in visual as well as in physiotherapy. Since the lesions are complicated, therapies have to be planned together with the child's neurologist. Actually, they can be seen as an important part of the neurological rehabilitation. Without ophthalmologic input training of visual functions seems to become repetition of eye movements and showing of pictures even if there might not be any information about picture perception. Pictures are used also in communication of these children, who have not been able to respond during measurement of visual acuity as grating acuity and contrast sensitivity with Hiding Heidi test.
Despite the very limited visual functions measurable in these children they need to have proper glasses and well structured environment so that there is a possibility to perceive some structures and, perhaps, use that information to recognise the place also via vision.
The new game-like tests that are now possible on computer screen may help us to learn more about visual functions in both these severely multi-impaired children and in very young infants.
In the assessment of vision of these children we record whether there are any responses to:
- the standardised fixation targets,
- any favourite object,
- tester's face,
parent's face. And if so, at which distance, whether the room lights need to dimmed and the object/person in spot light, how long the fixations are and the type of fixation, central, perifoveal or peripheral viewing with variation in fixating area.
to:
- illuminated small targets shown by the tester
- or held by the child him/herself alone or supported
lightbox with contrasting broad lines or picture of a face, distance from lightbox
following movements of eyes or head to the above mentioned objects
directions of movements possible: horizontal, right/left, vertical, diagonal, circular
saccades, elicited by which objects, to which directions, crossing midline
Presence of nystagmus, deviation of gaze, supranuclear palsies. Visual field by confrontation method using objects that were found interesting.
These findings do not describe vision well enough but are good to make in the beginning of therapy. During the therapy, observations are made during feeding, bath, dressing etc. on whether the child seems to recognise the situation and how the child experiences it.
If multisensory room is used, it should be assessed in terms of visual sphere, contrasts and luminance level. Many multisensory rooms that are pleasant to the personnel designing them have nearly no visual information for a severely visually impaired that would make sense and give structure to the place.
The time of these children must be very long - although many of them sleep a major part of the day - so it would be good to create entertaining and teaching materials for each child. These materials would allow further observations on what the child may see and remember.