14. THE UNTESTABLE CHILD
Children who are difficult to test are often said to be "impossible to test". This expression is used in a varying way. An ophthalmologist who is not accustomed to test young children may use this phrase when a nine year old child with Down syndrome does not know the names of numbers in a usual line test for adult persons. Then a wrong test has been used. Usually the phrase depicts a situation that the child does not respond to any of the routine test situations used in paediatric ophthalmology. This is not quite correct either. Routine tests have been chosen for measurement of visual functions in well responding children. When they do not work, we need to create new tests and test situations. Giorgio Porro calls such test situations "ethological analysis of visual behaviour". I usually call them "special tests" chosen in each case separately. Some test situations are so common that they have a name, like the 'Disco Heidi' or the 'Christmas beads' or the 'Black light balls'.
Most children can be tested for at least some visual functions but there are also children who do not respond in any of our usual or special test situations, yet we have a feeling that the child is not blind. Most often it is not possible to explain why there is that 'gut feeling' that the child sees something. Such children require repeated observations in varying postures during different time of the day by their therapists and parents and regular video recordings that are analysed by the low vision team.
Children who seem to be unresponsive to visual information, may respond poorly in the other modalities as well. Often the child has major brain damage due to either near drowning, encephalitis or traffic accident. Motor functions are very limited, often eye movements and swallowing are the only motor functions that the child has and even they do not seem to be controlled by the child. Eye movements are slow, aimlessly roving without obvious fixations at any objects or persons.
Loss of fixation does not prevent seeing. We see the room as a stable image when our gaze shifts from one fixation to the next or follows a slowly moving object. Whether the damaged brain can filter the stable image from the constantly changing visual information, we cannot assess today.
Clinical examination has usually tried to examine visual functions with VEP, ERG and by measuring several reflexes and described the structure of the eye in detail.
VEP, Visual Evoked Potential, measures the time needed for transfer from the retina to the visual cortex, mainly in the central 10-15 degrees. If VEP is extinguished, it does not mean that visual information does not reach visual associative functions. Visual information may be available to many visual and visuomotor functions although not recorded in a routine measurement of VEP. These functions are either subcortical or cortical and receive information through pathways other than the retinocalcarine pathway and the primary visual cortex.
ERG, electroretinography, measures electric potentials in the eye after specific stimuli. ERG may be nearly extinguished yet visual functions may be normal. On the other hand ERG and other functions in the eye may be normal but the information is lost on its way to the brain.
Clinical findings may give useful information about possibility to see but for example, detachment of the retina may seem to be total and thus the eye should be blind yet the infant responds to strong visual stimulation.
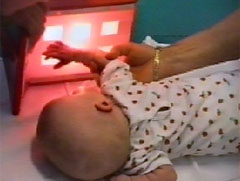
When an infant has severe brain damage and is unresponsive to visual stimulation during clinical examination, strong visual and tactile stimuli can be used to elicit responses. Since there is a danger of overstimulating, the child's condition must be closley observed. More on this baby in Chapter 12, 0-3 months.
In several cases of coloboma the structure of the retina and the optic nerve have been so abnormal that it is hard to believe that the infant can have useful vision.
Pupillary and blink reflexes are sometimes described as a part of "functional vision". Visual information used for these reflexes does not reach cortex, these reflexes are subcortical reflexes and may be present when posterior visual pathways, both the retinocortical and the tectal pathway are damaged.
In case of a non-responsive child we need to observe whether there is any changes in the child's behaviour or basic function that could be related to changes in the environment. Often we have to record breathing and pulse for long periods to find a change that coincides with auditory, tactile or visual information or a change in position. This does not yet prove that there is causal relationship and that the change is related to subjective perception of sensory information. The effect may be at a lower level in the brain.
Recording of pulse is important when strong sensory stimuli are used. Since the inhibitory mechanisms may not be effective, the stimulus may cause an abnormally strong arousal in the brain if it is suddenly transferred through the damaged pathways. Stimuli like the Disco Heidi or loud music with beating rhythm should be used only while carefully observing the child's behaviours.
During the first weeks after the trauma or infection the child may be functionally blind. Assessment and activation should be repeated as a part of physiotherapy to find out whether the neural networks have recovered enough to allow some transfer of information within one or several modalities. Plasticity of the neural networks is our hope and often leads to some function, sometimes to near normal function in a few functional areas.
During the therapy the therapist has an opportunity to become familiar with the child's responses and is thus able to also observe the weak responses to visual stimuli if or when they appear. On the other hand (s)he can confirm the finding that responses to visual stimuli do not occur in any posture even if the child seems to be at a high level of wakefulness. Some of these children remain functionally blind and need to be treated like blind children using tactile and auditory cues to inform them of what is going to happen. The appearance of responses within other senses but not to visual information confirms the diagnosis of blindness. However, it should be stressed even then that the long visual pathways may require a longer time to grow and to form new networks, so visual stimulation combining it with tactile and auditory information should be continued for months.