
#253300
A preferential looking test

In adults visual acuity is measured as "recognition acuity", which uses standard line tests. This type of test cannot be used in examining infants and children with multiple impairments. Instead of recognition visual acuity, grating acuity is measured with grating acuity tests either as detection or discrimination acuity. LEA GRATINGS test is a detection test.
In the LEA GRATINGS test, the infant or child detects the presence of parallel lines of decreasing width, a task simpler than recognizing optotypes. When a striped pattern is presented in front of an infant simultaneously with a gray surface of the same size and luminance, the infant is likely to look at the striped pattern because there is more to see than on a gray surface. What the child sees on the grating cannot be known. From children who can describe what they see we have learned that the lines on gratings can be seen distorted, only in a small part of the grating or the lines are so distorted that no lines are perceived.
The LEA GRATINGS test uses paddles to present gratings.
The handle allows the tester to hold the test easily.
The gratings are defined by the frequency, i.e., the number
of pairs of black-and-white stripes or cycles, within one
degree of visual angle. When grating is printed on a surface,
it can be defined also as the number of cycles per centimetre
of surface.
Infants and children at an early developmental level may
not respond to stimuli placed at 57 cm distance. Their
visual sphere may be limited to less than 30 cm (~ 1 ft).
When the gratings are held at half the 57 cm distance, the
number of cycles per degree (cpd) is half of that at 57 cm.
If the infant's response can be elicited only at 15 cm
(~ 1/2 ft), 1/4 of the original distance, the frequency
of the grating is 1/4 of the value printed on the test.
If the child responds to the stimuli at about 1 meter
(exactly 114 cm or ~ 4 ft), the grating acuity values
are twice the value printed on the test.
In the examination of infants it is advisable to choose test distances that are parts or multiples of 57 cm, i.e.
28 cm, 43 cm, 85 cm or 115 cm. Longer distances are rarely used.
Infants at the age of 8-12 months may have had their immunisation injections and learned that unknown people can be friendly and nice for a while but then they stick. These infants look worried as long as the tester is within her arm’s length from the infant and relax when the measurement is made at 115 cm distance.

The 1 cpcm grating is placed at 57 cm and at 114 cm from the camera. At the 57 cm distance the grating is an 1cpd stimulus and at the 114 cm distance the same grating is a 2 cpd stimulus. The distance of 57 cm is derived from the formula 2 p r. A circle has 360° and the circumference of a circle is equal to 2 p r (where r = the radius). In this case, "r" is equivalent to the distance between the child’s eye and the paddle. If the circumference of a circle measures 360 cm, then each degree of angle subtends to a distance of 1 cm on the circumference. The radius of such a circle, r, is then : r = 360 cm / 2 p = 57.2 cm.
Instructions
Make sure the background setting (including your clothing) is either evenly light gray or even dark colour to avoid patterns that could distract the infant. If the infant's visual sphere is limited, the surrounding visual information does not affect the child. However, these children are often disturbed by even weak noises and uncomfortable or unusual body postures.
Start with the coarsest grating. Show the infant the grating simultaneously with the gray stimulus. Then show every other grating in succession.
If the infant responds to the 0.25 and the 1.0 cpcm grating, but not to the 4.0 cpcm grating, present the 2.0 cpcm grating. The threshold is found quickly before habituation occurs. If the infant or child seems to lose interest, show a face figure (#253100 paddle) or colourful toys to motivate the infant to respond again.
PRESENTATION OF THE STIMULI
The measurement is based on observing the child's eye movements
when the grating paddles are presented to the child.
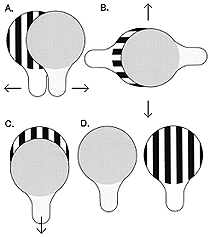
Different ways to present the LEA GRATINGS to children. The grating is kept behind the grey surface while moving it in the midline to the testing distance. When the grating and the grey surface are moved in opposite directions (A-C), motion perception is an additional factor in perception of the grating. When the grating and the grey surface are kept motionless (D) in front of the child, which resembles presentation of the Teller Acuity cards, motion perception does not affect the test situation.
When the grey surface and the grating are moved in opposite directions, some children with brain damage look confused and do not follow the movement of the grating but make a quick shift of gaze to the grating when it stops. This may be a sign of difficulties in seeing moving objects. On the other hand, some children have normal tracking movements, either eye movements or a combination of eye and head movements, but look surprised and confused when the grating stops. They may not have visual functions to perceive objects that stand still. Both observations need to be confirmed in other test situations.
The result is reported as “responded to ___ cpcm grating at a distance of ___ cm/inches”. This result should not be called grating acuity since we have no proof of how the infant has seen the test lines. We have not measured the true grating acuity, only a response to look at the lines. By reporting the cpcm value of the grating and the distance you also convey information on the infant’s visual sphere.
When explaining the results to people who are not familiar with grating measurements, you can show the grating that the infant or child responded to and say: "As you saw, your child could respond to these fine lines at this distance. This kind of grating is called .. (eg 2 cycles per cm, which means that there are two pairs of lines in each centimeter of the surface)." If you explain this well, the people will understand grating acuity much better than they will ever understand optotype acuities.
What is normal at different ages?
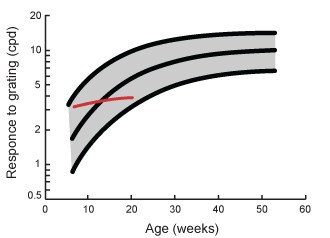
The drawing above shows the range of reactions of normally developing infants at different ages. Values that are clearly below the lower line are highly likely to be abnormal (except when the infant or child was tired or fuzzy). Values that are above the upper line are likely to be good normal values. Values within the range of normal are normal but do not mean that vision would be developing normally.
If an infant’s responses were in the upper normal range in the beginning and stayed at that level, did not improve with time (the red nearly horizontal line), visual development is not normal. This is an important finding, which should lead to further investigations.
In the graph the value on the Y-axis is cpd because that is the summary information of results of tests where test distances varied. The values are thus approximate. (Two values “3 cpd at 20 weeks” are not a truly same values if one measurement was made at 28 cm and another at 57 cm.)
[ Instructions I Paediatric Vision Tests I Vision Tests ]
This document was last modified on