
The Teller Grating Acuity Cards can be used to measure grating acuity in infants and children at early developmental levels. This is my oldest video recording of the Teller Acuity Cards during examination of an infant at the age of 8 months. The card with the grating at the one end and a grey area at the other end is presented to the infant and the tester looks through the peep hole to see, whether the infant fixates the grating. The fixation is taken as a sign of detection of the grating.
(This video was taken when I was assessing the Teller Acuity Cards in 1980s. It is rare to succeed in measuring the binocular value and the both monocular values in one session. Note that there is also an observation of normal auditory response, when a small instrument is dropped on the floor.)

Measurements of grating acuity with the LEA GRATINGS and contrast sensitivity with the Hiding Heidi test are quick. The infant follows the grating and the low contrast face picture with his gaze by turning his head. The response is easy to notice on the face of a normally developing infant at the age of three months. Assessment of multihandicapped infants is more difficult.
If you observe a social smile like that of this infant as a response to the smiling Heidi face, in that brief moment you observe visual functions, emotional functions and motor functions.

It should be kept in mind that grating acuity measures function in a much larger area of the visual field than optotype acuity. If there is loss of foveal function or central scotoma due to pathway damage, most of the grating may be well visible and the infant/child may respond to quite fine gratings.

The difference of the values of grating acuity and optotype acuity may be as extreme as in this case, where optotype acuity is barely measurable, in the range of 20/2000 (0.01, 6/600), grating acuity 6cpd (cycles per degree) and contrast sensitivity at the lower spatial frequencies close to normal values at the age of five years.

Measurement of grating acuity and assessment of contrast sensitivity with the Hiding Heidi test requires either following movements or saccades and fixation on a target long enough so that it can be noticed.
It effectively demonstrates to the parents the contrast level and the distance that are available for communication.

As said before, we need to know also refraction and accommodation to arrange communication at the distance where the infant sees the images best.
(Video 1)
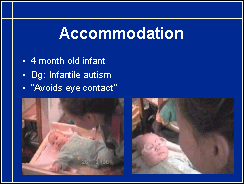
If an infant cannot accommodate, eye contact may not develop normally and early interaction may look as pathologic as in this case where the infant had been diagnosed as having infantile autism because she "avoided eye contact".
(Video 2)
This infant did not focus her eyes even when accommodative toys were used. When accommodation was compensated with "reading glasses" that make the image clear at the distance of one foot, the baby's reaction was immediate - as you will see.
The �reading glasses� are fitted for a communication distance of about 30cm (one foot); therefore the power of the lenses is +3 dioptres more plus than the basic refraction of the infant.

When an infant has infantile spasms and therefore strong medication to prevent seizures there may be no active looking at objects and no eye contact. This infant did not focus her eyes so near correction glasses were used. Notice the hypersensitivity of her head when the glasses are put on. After a moment the infant "woke up" and for the first time in her life looked at a face with good eye contact.
These two examples demonstrate the importance of good quality image for communication. In other children the response may not be as quick and obvious as in these two cases and may require several training sessions before the infant/child becomes aware of the change in image quality.

If an infant has poor vision and hearing, in this case due to a large coloboma in both eyes and abnormal ears, early interaction requires a lot of support. You see that the mother guides the little hand to feel the vibration of the vocal cords and movements of her lips to make the infant aware of the complex activities during communication. Videos like this are an important tool to teach the parents and caretakers and to demonstrate them that the infant is interested in interaction. Because of the coloboma, the infant seems to look at the hair of an adult when he actually is looking at the eyes of the adult person.
In western countries we are very sensitive to deviations from the normal eye contact and often interpret them as signs of lack of interest in communication. Negative reactions like this need to be knowingly avoided. The infant or child usually does whatever he can to participate in communication. The problem is that of an adult who does not understand the communication of the child.

When it is likely that contrast sensitivity may not be normal, it can be roughly assessed by using the Hiding Heidi test within the visual sphere of the infant. In this case the infant responded to 25% picture of the face picture, not to the lower contrasts, which means that the parents must have heavy make up to be seen by the infant. Otherwise we pretend having visual communication with the infant but actually are not giving anything. Have you considered that while we do not whisper to hearing impaired infants, we often "whisper visually" to visually impaired infants and children.

To become visible we may increase contrast on the adult people's face by using make up, lip and eye liner and fathers may have short moustaches. We can improve the quality of visual information by being close to the infant (=geometric magnification) and by supporting it with tactile information from the vocal cords and lips (=Tadoma).

To repeat, for communication and interaction we need to measure grating acuity and contrast sensitivity, need to know the refractive error and accommodation of the infant and test whether near correction supports early interaction.
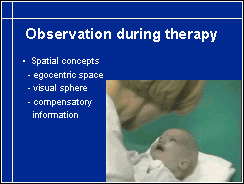
Therapists have an important role in the observation of development of visual functions and in training them. You see how gently and skilfully the therapist guides the infant to explore his feet tactily and visually. As a part of the therapy sessions, following movements can be tested better than during a clinical examination. (The day before this infant had been diagnosed as totally blind at the local university hospital because he did not respond to any of the usual fixation targets.)

During the first year especially, but as a part of all later assessments, we need to observe all these functions: motility, nystagmus, fixation, infant's behaviour during interactions; and measure grating acuity, contrast sensitivity, visual field and visual adaptation and when the infant has good following movements observe also visual anticipation.

With visual anticipation we mean that the infant moves his eyes with correct speed even if the target disappears behind an obstacle and then reappears on its other side. This means that the infant has the concept of object permanence, can perceive the speed of movement and continues the eye movement with an anticipation of seeing the object when it appears from behind the obstacle. At the age of four months anticipation is just emerging.

At the end of the first year of life we can start making observations on the infant's ability to recognise. Re-cognise means that there is a template in the memory of the infant and it can be used to compare with the object or person present. If an infant does not recognise family members when they are quiet but responds to them when they start talking, vision needs to be thoroughly assessed. It may be that the image is so blurred or patchy that the infant can recognise facial features first quite near or it may be that the infant has not developed the specific cortical function of recognition of faces. Measurement of grating acuity, contrast sensitivity and visual sphere give information about the function of the anterior part of the visual system, the quality of the image. Observations on the role of visual and auditive information in interaction help us to make the diagnosis of problems in cognitive vision. If an infant does not recognise people, communication in a group of toddlers and still in kindergarten will be problematic and requires special attention, a support person who functions as an interpreter.
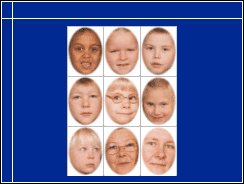
Pictures of family members and peers can be used to test recognition of faces. First we need to know that the child can see the pictures well enough to match two copies of each picture. When this is possible, we can ask "Who is in this picture?" Pictures should not have any other details but the face because all details will be used for comparison and recognition. (See also Transdisciplinary Assessment of Vision II, slide 21.)

Every delay in reaching a developmental milestone should be a 'red flag' and should lead to a careful assessment. One of the most sensitive functions to observe is the eye contact. If an infant does not have normal eye contact but seems to look past or above the eyes of the adult person, it could be a sign of a central scotoma.
If an infant has unusual eye movements, nystagmus or strabismus, the eyes and the visual pathways need to be examined. It is still quite common that the eyes are examined in detail but refraction is not measured and/or lesions of the posterior pathways are not considered. If an infant's visual behaviour deviates from the age appropriate then also cognitive vision losses need to be carefully evaluated. In the diagnostic work, videos taken in therapy and play situations and during interactions often help to pinpoint the nature of an infant's problem.

Over the years I have collected a great number of video observations on children with different kinds of vision problems. Some of the video sequences are on my web pages and a larger collection of them is on a CD called LH Materials 2001. The videos have been very helpful in clinical and functional assessment of many children and may give you ideas on what to look for in the infants and children whom you take care of. Observations during daily activities are and will be important. Even if we have fine clinical tests, functional assessment is still the foundation for early intervention and special education needs. In this work the role of teachers and therapists is of great importance.